Breast Cancer Detection & Diagnosis
Breast Cancer
Screening for Breast Cancer
An important step women can take to protect their health is to get a mammogram. It is the American Cancer Society's primary recommended breast cancer screening method. Because there are no symptoms of breast cancer at its earliest stages, this screening test saves lives.
Related Reading:
Are There Early Signs of Breast Cancer?

Mammograms Detect Cancer Before It Can Be Felt
A mammogram is an X-ray picture of tissue inside the breast. It can often show a breast lump before it can be felt. They can also display a cluster of calcium specks called microcalcifications. Lumps or specks can be from cancer, precancerous cells, or other conditions. Further testing is needed to find out whether cancer cells are present.
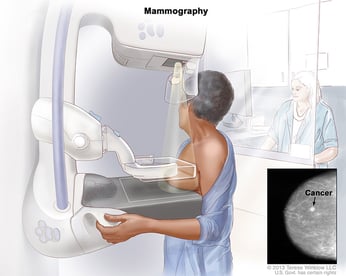
Women should get regular screening mammograms to detect breast cancer early— even before they have symptoms. According to the American Cancer Society:
- Women between the ages of 40 to 44 have the choice to start yearly mammography
- Women aged 45 to 54 are recommended to receive a mammogram every year
- Women age 55 and older can switch to having a mammogram every two years or continue yearly screening if they choose
- Women under the age of 40 who have risk factors for breast cancer should ask their healthcare provider whether to have mammograms and how often to have them.
If the mammogram shows an abnormal area of the breast, your doctor may order more detailed images. Doctors use diagnostic mammograms to learn more about unusual breast changes, such as a lump, pain, thickening, nipple discharge, or change in breast size or shape. Diagnostic mammograms may focus on a specific area of the breast, offering more detailed views than traditional screening mammograms.
Related Reading:
Detecting Breast Cancer Early with 3-D Mammograms

Clinical Breast Exam
While it's not part of the American Cancer Society's primary breast cancer screening recommendations, a breast exam performed by a healthcare professional is a good idea during an annual office visit.
You may be asked to raise your arms over your head, let them hang by your sides, or press your hands against your hips as the provider feels various areas of the breast. Your nipples may be squeezed to check for fluid. In addition to looking for differences in size or shape between your breasts, your doctor will check your breasts’ skin for a rash, dimpling, or other abnormal signs.
Your healthcare provider also checks the lymph nodes near the breast to see if they are enlarged.
If a lump is present, its size, shape, and texture will be examined. Your healthcare provider will also check to see if the lump moves easily. Benign (noncancerous) lumps often feel different from malignant (cancerous) ones. Lumps that are soft, smooth, round, and movable are likely to be benign. On the other hand, a malignant lump is a hard, oddly shaped lump that feels firmly attached to the breast. Regardless, further tests are needed to make an accurate diagnosis.
Tests to Diagnose Breast Cancer
Other imaging tests may be ordered if an abnormal area is found during a clinical breast exam or with a mammogram. These can include:
Ultrasound
An ultrasound uses sound waves to create a picture of the breast tissue. The sound waves echo differently when bouncing off abnormal tissue and healthy tissue. An ultrasound can distinguish between a solid mass, which may be cancer, and a fluid-filled cyst, which is usually not cancer.
Breast MRI
An MRI uses magnetic fields to produce detailed images of the body. A special dye is given before the scan to help create a clear picture of possible cancer. This dye can be injected into a patient’s vein or given as a pill to swallow. A breast MRI may also be used after a breast cancer diagnosis. They are used to check for additional diseases or to determine how much the cancer has grown or spread. It may also be used before surgery to determine if chemotherapy is effectively shrinking the tumor.
Breast Biopsy
A biopsy is the removal of tissue to look for cancer cells. It is the only way to tell for sure if cancer is present. If an abnormal area is found during an exam or on a mammogram, you will likely need a biopsy.
Your doctor may refer you to a surgeon or breast cancer specialist for a biopsy. The surgeon or doctor will remove fluid or tissue from your breast in one of several ways:
- Fine-needle aspiration biopsy: The use of a thin needle to remove cells or fluid from a breast lump.
- Core biopsy: The use of a wide needle to remove a sample of breast tissue.
- Skin biopsy: The removal of a small sample of skin if there are skin changes on your breast.
- Surgical biopsy: The removal of a sample of tissue.
- An incisional biopsy takes a part of the lump or abnormal area.
- An excisional biopsy takes the entire lump or abnormal area.
- Image-guided biopsy: A needle is guided to the site of the abnormal growth with the help of an imaging technique, such as mammography, ultrasound, or MRI. An image-guided biopsy can be done using a fine needle or core needle (see above), depending on the amount of tissue being removed. Imaging tests may also be used to help conduct a biopsy on a lump that can be felt, to help find the best location.
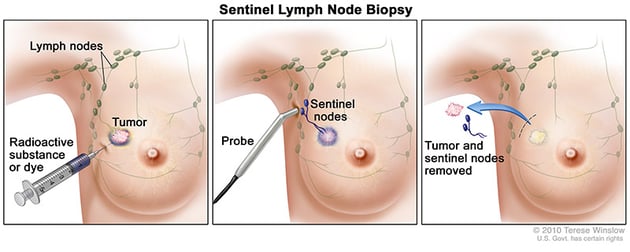
- Sentinel lymph node biopsy: To determine if there is cancer in the lymph nodes near the breast, a surgeon injects a radioactive substance and/or a blue dye near the tumor to locate the position of the sentinel lymph node. Once the sentinel lymph node is found, the surgeon makes a small incision in the overlying skin and removes the node. The sentinel node is then checked for the presence of cancer cells by a pathologist. If cancer is found, the surgeon may remove additional lymph nodes, either during the same biopsy or during a follow-up surgical procedure. This procedure is usually done at the same time the primary tumor is removed. However, the procedure can also be done either before or after the removal of the cancer.
A pathologist will check the removed breast tissue or fluid for cancer cells. If any are found, the pathologist will be able to determine what kind of cancer is present. The most common type of breast cancer is ductal carcinoma, a type of breast cancer that begins in the cells lining the breast ducts. Another type is lobular carcinoma is another type, which starts in the lobules of the breast.
Lab Tests with Breast Tissue
If you are diagnosed with breast cancer, your doctor may order special lab tests on the removed breast tissue:
- Hormone receptor tests: Some breast cancer tumors need hormones to grow. These tumors have receptors for the hormones estrogen, progesterone, or both. If the hormone receptor tests show that the breast tumor has these receptors, then hormone therapy is usually part of the recommended treatment plan.
- HER2/neu test: HER2/neu protein is found on some types of cancer cells. This test shows whether the tissue has too much HER2/neu protein or too many copies of its gene. If the breast tumor has too much HER2/neu, then targeted therapy may be a treatment option.
- Grade: Grade refers to how different the cancer cells look from healthy cells, and whether they appear slower-growing or faster-growing. If the cancer looks similar to healthy tissue and has different cell groupings, it is called “well-differentiated” or a “low-grade tumor.” If the cancerous tissue looks very different from healthy tissue, it is called “poorly differentiated” or a “high-grade tumor.” There are three grades: grade 1 (well-differentiated), grade 2 (moderately differentiated), and grade 3 (poorly differentiated).
- Molecular testing of the tumor: Other laboratory tests may be run on a tumor sample to identify specific genes, proteins, and other factors unique to the tumor. Your doctor may recommend testing for various molecular features if you have locally advanced or metastatic breast cancer.
- Genetic testing: Genetic factors cause some breast cancers. Genetic testing will determine whether there are any harmful BRCA1 or BRCA2 gene mutations.
- Genomic testing: These tests are used to look for specific genes or substances made by the genes, called proteins, that are found in or on cancer cells. These tests highlight the unique features of each individual’s breast cancer. Genomic tests can also help estimate the risk of the cancer coming back after treatment.
It may take several weeks to get the results of these tests. While the wait can be hard, your doctor must go over these test results thoroughly to determine the best breast cancer treatment option.
Blood Tests
Blood tests, which may be done before or after surgery, could also be needed. There are different types of blood tests, which include:
- Complete blood count (CBC): A CBC is used to measure the number of specific cell types, such as red blood cells and white blood cells, in a sample of a person’s blood. This test can determine whether or not your bone marrow is functioning as it should.
- Blood chemistry: This test evaluates how well your liver and kidneys are working.
- Hepatitis tests: These tests are occasionally used to check for evidence of prior exposure to hepatitis B or hepatitis C. If an active hepatitis B infection is present, you may need to take a particular medication to suppress the virus before receiving chemotherapy. Chemo can cause the virus to grow and damage the liver if this medication is not taken.
Once all diagnostic tests are completed, your doctor will go over the results with you. If the diagnosis is cancer, these results also help the doctor describe the disease, which is done through staging. Depending on the stage of breast cancer, additional imaging tests may be recommended. If there is a suspicious area found outside of the breast and nearby lymph nodes, additional biopsies of those areas may be needed to find out if it is cancer.
Breast Cancer Care is Available at Willamette Valley
If you or a loved one is newly diagnosed with breast cancer, the oncologists at WVCI will walk you through every step of the treatment process and the plan that’s right for you. Appointments are available at our locations in Albany, Corvallis, Eugene, Florence, and Newport, Oregon, with a breast cancer doctor.
